
Latest Blogs
The physicians and staff at Prestige understand that being injured in an auto accident can be extremely stressful for you and your family.
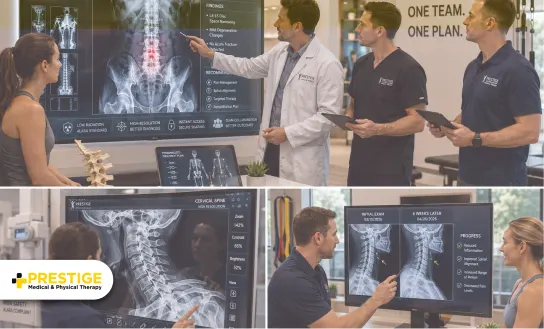
Clinical and Safety Benefits of Digital Radiography in Multidisciplinary Care
Healthcare professionals analyzing digital X-ray imaging and spinal scans with a patient to improve diagnostic accuracy, treatment planning, and collaborative multidisciplinary care.
Read More →
How Integrated Medical Services Create a Personalized Treatment Plan for Faster Healing
Recovery after an injury requires more than a single doctor. Our integrated medical services at Prestige ensure you receive a personalized treatment plan for faster healing by addressing the root cause of your pain immediately.
By bringing all specialists under one roof, we eliminate the gaps in care that often slow down recovery times. If you are recovering from an auto accident in Florida, our team works together to restore your health and get you back to your normal life quickly.
1. How Integrated Medical Services Develop a Customized Healing Plan
Most traditional medical offices focus on one specific symptom at a time. This often fosters a one size fits all approach where every patient receives the same generic stretches or pills.
At our Tampa facility, we believe your body deserves better. We use a patient-centered care model that treats you as a whole person rather than a set of symptoms.
Our team consists of specialists in Internal Medicine, Chiropractic Care, and Physical Therapy. These professionals play a crucial role in your journey.
They communicate daily to ensure your treatment plan evolves as you heal. This interdisciplinary strategy allows us to provide effective treatments that adapt to your specific biological needs.
2. Why We Focus on Root Cause Analysis in Integrated Medical Care
We start each case by thoroughly reviewing your health history and current physical condition. This is called root cause analysis in medicine.
Precise Diagnostics for Accurate Injury Mapping
We use modern diagnostics to build your health profile. This includes digital imaging, blood work, and functional movement screens. Our team uses Electronic Health Records to share these results instantly across all departments. This ensures that your chiropractor and your physical therapist are looking at the same data.
Effective Treatment Plans Instead of Quick Fixes
We incorporate functional medicine protocols to look at how different systems in your body interact. For example, we might examine how inflammation in your gut affects tissue repair in your spine. This level of detail helps us personalize treatment to your unique biology.
3. How Multidisciplinary Care Reduces Recovery Time
When you visit multiple different clinics, your care becomes fragmented. You might spend weeks waiting for a referral or a phone call between offices. We solve this problem by housing our entire team in one Tampa location.
Our Collaborative Care Coordination Make Faster Recovery
Our collaborative care coordination means your doctors talk to each other every day. If your chiropractor finds a specific spinal misalignment, they tell your physical therapist immediately. The therapist then adjusts your exercises to support that specific area. This real time adjustment reduces the risk of further injury and shortens your recovery time.
Our Physical Therapy and Chiropractic Care Combo
Physical therapy and chiropractic care work better together. Chiropractic adjustments align the structure of your spine. Physical therapy then strengthens the muscles around that structure to keep it in place. This synergy is a pillar of our holistic healthcare approach.
Also read: Neck and Back Pain Relief Without Surgery: Proven Therapy and Chiropractic Approaches That Work
4. Biological Processes and Faster Healing at a Cellular Level

Healing is a biological sequence that requires the right environment. Our goal is to trigger cellular regeneration and maintain homeostasis within your body. This balance is essential for long-term healing, as noted by the Mayo Clinic.
We Control Inflammation for Rapid Tissue Repair
After an auto accident, inflammation is your biggest enemy. While some inflammation is natural, chronic swelling prevents oxygen from reaching damaged cells. We use specific medical intervention and nutritional science to control this process. By reducing swelling quickly, we allow the tissue repair phase to begin sooner.
Precision Medicine and Lifestyle Factors
We use principles of precision medicine to tailor your recovery. This includes looking at lifestyle factors like your sleep habits and stress levels. Our team may even use biofeedback to help you understand how your nervous system responds to pain. This data allows you to make informed decisions about your daily routine.
5. Personalized Treatment Plan for Auto Accident Injuries in Tampa, Florida
The roads in Tampa see thousands of accidents every year. If you are involved in a crash, Florida law requires you to seek medical attention within 14 days to protect your insurance benefits.
Our Specialized Care for Whiplash and Spinal Injuries
We specialize in treating injuries common to car accidents. Whiplash often involves both bone and soft tissue damage. A multidisciplinary medical team is essential for these cases. We combine medical symptom management with active rehabilitation to ensure your spine heals correctly.
We Improve Your Overall Quality of Life
Our mission goes beyond just fixing a single injury. We want to improve your overall quality of life. This involves a long term view of your health that includes preventive medicine.
6. The Biopsychosocial Model of Care

We use a biopsychosocial model, a framework recognized by the American Psychological Association (APA) that considers your physical, mental, and social health. We believe that a patient who actively participates in their care sees better clinical outcomes. When you take an active role, you are more likely to stay healthy in the long run.
Helping Patients Be Actively Involved
We educate you on your treatment options so you can choose the path that fits your life. You are not a passive observer in our clinic. You are the most important member of the team. When a patient actively participates, they experience improved patient satisfaction and better physical results.
Wholehearted Approaches to Chronic Disease Management
Even if you came to us for an injury, we look for ways to boost your total health. We use holistic approaches to address chronic disease management. This might include nutritional science to help you lose weight or psychology to help you manage chronic pain stress. These extra steps ensure that your body is strong enough to resist future ailments.
Also read: Does Physical Therapy Actually Work for Chronic Back Pain?
Start Your Personalized Recovery Today

Healing from an injury does not have to be a slow or confusing process. By choosing integrated medical services, you ensure that every specialist is working toward the same goal. We provide the tools, the team, and the technology to get you back on your feet. Our personalized care plans are designed to help you recover faster and stay healthy longer. If you are ready to move past your pain, our Tampa team at Prestige is one call away.
Contact: (813) 243-2500
Website: www.prestigemedpt.com
Frequently Asked Questions
Does insurance cover integrated medical services at your Tampa clinic?
Yes, most major health insurance plans and Florida Personal Injury Protection cover our multidisciplinary treatments.
How long will it take for me to see results from my treatment plan?
While every case is unique, many patients report feeling significant relief within the first two weeks of our integrated care.
Do I need a referral from my primary doctor to visit Prestige Medical?
No, Florida law allows you to seek chiropractic and physical therapy services directly without a prior referral.
What should I bring to my first appointment after a car accident?
Please bring your insurance information, any police reports from the accident, and any previous imaging or medical records you have.
Can I receive chiropractic care and physical therapy on the same day?
Yes, we often schedule these treatments back to back to maximize the synergy between spinal alignment and muscle strengthening.
What happens if my pain returns after I finish my initial treatment plan?
We offer long term wellness checks and preventive medicine strategies to ensure your body remains stable and pain free.
Disclaimer: This article provides general information and does not constitute medical advice. Please contact Prestige Medical and Physical Therapy for personalized diagnosis and treatment.
Read More →
Hip Joint Pain Physical Therapy Exercises for Post-Injury Recovery
Recovering from a hip injury is a journey that requires patience and a strategic approach. The hip joint is a central pillar of your body and handles immense pressure during every step you take. When you suffer from an injury, your mobility can drop significantly. Many people find that even getting out of bed causes a sharp sense of pain and stiffness.
Our specialists at Prestige Medical Physical Therapy focus on restoring your movement through evidence-based methods. Our goal is to move you from a state of limitation back to your normal physical activity level.
Whether your discomfort stems from sports injuries or general wear and tear, a structured plan is vital. Physical therapy exercises for hip pain are not just about movement. They are about rebuilding the foundation of your lower body. By following a guided exercise program, you can address the root cause of your discomfort rather than just masking the symptoms.
1) Hip Joint Pain and Recovery
The hip is a ball-and-socket joint that relies on a complex network of ligaments and tendons. When an injury occurs, these structures can become inflamed. In some cases, a fluid-filled sac called a bursa becomes irritated, leading to a condition known as bursitis. This can make the entire area feel tender to the touch.
(I) Common Causes and Medical Conditions
Many different health conditions can lead to persistent hip issues. Arthritis is a frequent culprit, often categorized as a chronic condition that requires long-term management. According to the Centers for Disease Control and Prevention, roughly one in four adults in the United States has been diagnosed with some form of arthritis. This diagnosis often brings about significant pain and stiffness in the joints.
Other medical conditions, like labral tears or tendinitis, are also common after sudden movements or falls. Statistics show that more than 300,000 older adults are hospitalized for hip fractures each year in the U.S.. Regardless of the specific cause, the primary focus of recovery is always on protecting the joint while rebuilding strength.
(II) The Role of Blood Flow in Healing
Healing cannot happen without proper circulation. Increased blood flow delivers essential nutrients and oxygen to the injured tissues. Movement is the most effective way to stimulate this process. When you engage the surrounding muscles, you create a pump-like effect that clears out inflammatory markers.
Prestige Medical Physical Therapy experts emphasize that movement is medicine. Even small, controlled movements can prevent the joint from becoming frozen or excessively stiff. This is why we start with low-impact stretches before progressing to more strenuous tasks.
2) Prepare for Your Exercise Program

Starting a new routine can feel overwhelming when you are in pain. It is important to know that you are not alone in this process. Before you dive into specific movements, you need to understand the baseline of your physical health.
(I) What to Expect During Your Initial Visit
Your first step should always be a professional evaluation. This helps identify which specific muscles are weak and which ones are overcompensated. You might find it helpful to learn what to expect at your first physical therapy session so that you feel prepared for the assessment.
During this time, a therapist will look at your range of motion and your gait. They will ask about your history with sports injuries or any underlying health conditions. This information allows them to craft a treatment plan that is safe for your unique body.
(II) Managing Pain and Stiffness
It is normal to feel some resistance when you first start moving an injured hip. However, there is a big difference between a healthy stretch and a painful strain. The experts at Prestige Medical Physical Therapy suggest using heat or ice to manage discomfort before and after your sessions.
The goal of your exercise program is to gradually increase what your body can handle. We want to reduce the risk of re-injury by ensuring your form is perfect. Consistency is the key to turning a chronic condition into a manageable one.
3) Primary Physical Therapy Exercises for Hip Pain

The following exercises are commonly used in post injury recovery. They focus on mobility, stability, and strengthening the muscles that support the hip joint.
(I) Mobility and Range of Motion
Before you can build strength, you must ensure the joint can move through its natural path.
Seated External Hip Rotation: Sit in a sturdy chair with your feet flat on the floor. Cross your left leg so that your ankle rests on your right knee. Gently press down on your left knee until you feel a stretch in your hip. It is important to hold the stretch for 20 to 30 seconds. Repeat on the opposite side to ensure balance. This helps maintain the rotation needed for walking and climbing stairs.
The Butterfly Stretch
Sit on the floor with your knees bent and the soles of your feet touching. Hold your feet and gently lower your knees toward the ground. You will feel a stretch in your inner thighs and hips. Hold the position while taking deep breaths.
(II) Strengthening the Muscles
Once your mobility improves, you can start to strengthen your hip. This protects the bone and cartilage from unnecessary impact.
The Leg Raise
Lie flat on your back on a mat. Keep one knee bent and feet flat to support your lower back. Lift your left leg slowly until it is about 12 inches off the ground. Keep your leg straight throughout the motion. Hold the position for a second at the top. Slowly lower the leg back to the start position. Complete 10 repetitions and then repeat on the opposite side.Bridges for Glute Activation
Lie on your back with your knees bent and feet flat on the floor. Squeeze your glutes and lift your hips toward the ceiling. Your body should form a straight line from your knees to your shoulders. Hold the position for three seconds before you return to the starting position. This move is essential for stabilizing the hip joint during daily activities.
4) Beyond the Hip Joint
The human body is an interconnected web. Often, pain in one area is caused by a weakness in another. Hip pain frequently correlates with issues in the lower back or even the knees.
(I) Connection to Chronic Back Pain
If your hip is not moving correctly, your lower back often has to pick up the slack. This can lead to a secondary chronic condition in your spine. Many patients wonder whether physical therapy actually works for chronic back pain when their primary issue started in the hip. The answer is a resounding yes because physical therapy addresses the entire kinetic chain.
Research published by the National Institutes of Health indicates that patients who engage in physical therapy for musculoskeletal pain see a 50 percent reduction in the need for invasive surgeries. By strengthening the surrounding muscles, you take the pressure off both your hip and your back.
(II) Benefits of Chiropractic Manipulation
Sometimes, a joint can become restricted in a way that exercise alone cannot fix. In these cases, manual therapy can be very beneficial. You might consider chiropractic manipulation for everyday pain to help realign the joint and improve nervous system function.
Prestige Medical Physical Therapy often utilizes a multidisciplinary approach. Combining exercise with manual adjustments can accelerate your recovery timeline. This ensures that the hip joint is moving freely while the muscles are being trained to support it.
5) Progress to High-Impact Activity

The final phase of recovery is returning to the things you love. This might mean running, playing sports, or simply playing with your grandchildren.
Gradual Loading: You should not jump straight back into running. Start with fast walking or swimming.
Monitoring Symptoms: If pain and stiffness return after a session, it means you might need to scale back.
Occupational Therapy: If your job requires heavy lifting or long hours of standing, occupational therapy can help you adapt your movements to stay safe.
The National Health Interview Survey suggests that joint pain is a leading cause of work disability in the United States. By taking your exercise program seriously, you are protecting your career and your long-term independence.
Frequently Asked Questions
How often should I perform these hip exercises?
Most patients see the best results when they perform their stretches daily and their strengthening moves three to four times a week. However, you should follow the specific treatment plan provided by the team at Prestige Medical Physical Therapy.
Is it normal to hear a clicking sound in my hip?
A clicking or snapping sound can be common and is often just a tendon moving over a bone. However, if the click is accompanied by pain, it could indicate a labral tear or an issue with a fluid-filled sac. You should have it evaluated by a professional.
Can physical therapy help with age-related hip pain?
Yes, it is highly effective. Strengthening the muscles around the joint can significantly reduce the symptoms of arthritis and other age-related health conditions. It helps maintain your ability to perform daily activities without help.
When can I return to sports after a hip injury?
You can usually return to impact activity once you have regained full range of motion and your strength is equal on both sides. Your physical therapist will use specific tests to determine when you are ready to play safely.
Disclaimer: This article provides general information and does not constitute medical advice. Please contact Prestige Medical and Physical Therapy for personalized diagnosis and treatment.
Read More →
Essential Mobility Restoration Tips for Faster Recovery After Injury
An injury often feels like a sudden wall in the middle of a clear path. It disrupts your daily routine and affects your mental wellness. Most importantly, it distances you from the activities that bring you joy. Prestige Medical & Physical Therapy understands the frustration of a forced pause. We see the determination in our patients who want to return to their jobs and their families. Use of specific mobility exercises for injury recovery helps you handle the journey back to full health safely.
The road to restoration does not require a choice between total stillness and painful exertion. True healing happens in the space between those extremes. We believe that informed patients achieve better outcomes. By understanding how your body heals, you can take an active role in your own progress.
1) The Transition from Rest to Active Restoration
For decades, the standard advice for any injury was total rest. Doctors recommended staying in bed and avoiding all movement. Modern medical science now offers a different perspective. While the initial stage of an injury requires protection, prolonged inactivity can actually hinder your progress.
"The CDC reports that regular physical activity provides immediate health benefits. It reduces the risk of chronic conditions and improves the healing process for various physical ailments."
(Source: Centers for Disease Control and Prevention)
Benefits of Controlled Motion
Movement encourages blood flow. It delivers oxygen and essential nutrients to the damaged tissues. It also helps flush out the waste products of inflammation. We refer to this as active recovery. However, this movement must be controlled and intentional.
Avoidance of Muscle Decay
The goal of restoring motion is to regain the ability to move a joint through its full range without pain. This differs from simple stretch routines. Mobility involves strength and control. It ensures that your joints remain stable while you move.
Explore more: What to Expect at Your First Physical Therapy Session
2) Early Mobility Exercises for Injury Recovery and Health

The body is highly efficient. When you stop using a muscle group, the body begins to conserve energy by breaking down that tissue. This process is known as atrophy. It can start within just a few days of total inactivity.
"Data from the NIH indicates that musculoskeletal disorders are a leading cause of disability in the United States. Early intervention and movement based therapies significantly reduce lasting disability rates."
(Source: National Institutes of Health)
Nerve and Muscle Communication
Starting restorative drills early helps maintain the connection between your brain and your muscles. Professionals call this neuromuscular control. When you get injured, the nerves often stop communicating effectively with the affected area. Gentle motion drills keep those pathways open. They prevent the stiffness that often follows surgery or trauma.
Safe Motion Timelines
However, timing is everything. Our team monitors the inflammatory phase closely. Once the initial swell subsides, we introduce movements that challenge the tissue without causing further damage. This approach shortens the overall recovery timeline.
Related post: Neck and Back Pain Relief Without Surgery: Proven Therapy and Chiropractic Approaches That Work
3) Three Core Pillars of Functional Mobility Restoration After Injury
To build a solid foundation for your recovery, we focus on three specific areas of movement. Each pillar supports the others. Skip one can lead to imbalances that increase the risk of future injuries.
Joint Range Recovery
Range of motion refers to the distance and direction a joint can move. After an injury, scar tissue often limits this movement. We begin with passive movement. This means a therapist or a tool moves the joint for you. Gradually, we progress to active motion where you move the joint using your own muscle power.
Stability and Balance
A mobile joint is only useful if it is also stable. Stability comes from the ligaments and the small muscles surround the joint. We use balance drills and isometric holds to build this stability. These movements teach your body to stay aligned even when you are on the move.
Muscle Length and Elasticity
Flexibility involves the ability of your muscles to lengthen. We focus on functional flexibility. This means the muscles can lengthen while you perform a task. This prepares you for real life movements like reach for a high shelf or climb stairs.
4) Risks of Prolonged Rest and Inactive Injury Recovery

Choosing not to move carries its own set of risks. Beyond muscle loss, inactivity affects your cardiovascular health. It can also lead to secondary pains. For example, a person with a knee injury might develop back pain because they sit in an awkward position all day.
"The CMS highlights that physical therapy and active rehabilitation are cost effective ways to manage recovery. These methods often prevent the need for more invasive and expensive surgeries later in life."
(Source:Centers for Medicare & Medicaid Services)
Heart and Lung Health
We prioritize movement to keep your entire system healthy. A body in motion tends to stay in motion. By keeping the rest of your body active while the specific injury heals, you maintain your overall fitness. This makes the final transition back to your normal life much smoother.
Prevention of Compensatory Injury
When one part of the body stops moving, other parts overwork to compensate. This often leads to new injuries in unrelated areas. Proper motion drills ensure that the load remains even across your entire skeletal system.
5) Customized Injury Rehabilitation and Mobility Therapy Plans from Prestige Medical & Physical Therapy
Every injury is unique. A protocol that works for a sprained ankle will not work for a torn rotator cuff. This is why professional assessment is vital. Prestige Medical & Physical Therapy creates a roadmap specifically for your body.
"The HHS emphasizes the importance of personalized healthcare plans. Tailored interventions lead to higher patient satisfaction and better clinical results across all demographics."
(Source: United States Department of Health and Human Services)
Individual Healthcare Strategies
We use advanced diagnostic tools to measure your current capabilities. We then set realistic milestones. Our staff provides the feedback you need to know if you do a drill correctly. Form is more important than intensity.
Metric Based Progress Tracking
Doing a movement wrong can create a new problem. Doing it right under our supervision ensures your safety. We track every small gain to ensure you stay on the path toward your ultimate goal.
6) Listen to Your Body During Mobility Based Recovery
During recovery, you will feel many different sensations. Some are helpful. Others are warnings. We teach our patients how to distinguish between these signals.
Pain Scale Distinction
Discomfort is a normal part of the process. As you break down old scar tissue and stretch tight muscles, you will feel some tension. This is often a dull ache. However, sharp or stab pain is a signal to stop.
Realistic Recovery Timelines
We encourage you to be patient with yourself. Heal is not a linear process. You will have days where you feel strong and days where you feel stiff. Consistency over time produces the best results. We adjust your plan whenever your body needs a different approach.
7) Nutrition and Hydration Strategies to Support Tissue Repair and Mobility Recovery

Restore motion is not just about movement. It is also about what you put into your body. Your tissues need building blocks to repair themselves. Proteins and vitamins play a crucial role in the remodel of collagen.
"The FDA monitors the safety of supplements and medical foods used in recovery. A balanced diet supported by evidence based nutrition is fundamental to tissue repair and immune function."
(Source: Food and Drug Administration)
Nutrient Density for Cells
The body requires specific amino acids to rebuild muscle and tendon fibers. We recommend a diet rich in lean proteins and leafy greens. These foods provide the raw materials for cell regeneration.
Hydration for Joint Health
Hydration is equally important. Water keeps your joints lubricated. It allows the fascia to slide and glide easily. Dehydrate tissue is brittle and more prone to tear. We recommend consistent water intake throughout the day to support your restorative work.
Your journey toward wellness is a true partnership where our clinical expertise meets your dedicated effort. Prestige Medical & Physical Therapy holds the belief that movement is the ultimate medicine and the most reliable path to a life without limitations.
Contact Prestige Medical & Physical Therapy
Reach out to our multi-disciplinary team to start your custom path to health today.
Phone: (813) 243-2500
Address: 8313 W. Hillsborough Ave., Suite 330, Tampa, FL 33615
Website: www.prestigemedpt.com
Disclaimer: This article provides general information and does not constitute medical advice. Please contact Prestige Medical and Physical Therapy for personalized diagnosis and treatment.
Frequently Asked Questions
How do I know if I am ready for movement drills?
You are usually ready for gentle motion work once the sharp pain of the injury begins to fade. If you can move the joint even a small amount without intense pain, you can begin basic drills. However, you should always consult with a professional at Prestige Medical & Physical Therapy before starting a new routine. We ensure that your bones and ligaments are stable enough for movement.
How often should I perform my mobility sessions?
Consistency is more effective than intensity. We usually recommend short sessions performed several times a day. For example, doing five minutes of movement three times a day is better than one long session that leaves you exhausted. Frequent movement keeps the joint from stiffening up between sessions. Your specific plan will outline the exact frequency.
Can active recovery replace surgery?
In many cases, a dedicated movement and strength program can help a patient avoid surgery. This is especially true for joint issues related to wear and tear. Even if surgery is necessary, performing these drills beforehand can improve your outcomes. Professionals call this preparation before surgery. It makes your body stronger for the phase after the operation.
Read More →
Injury Rehabilitation: How Targeted Physical Therapy Speeds Up Recovery After Accidents and Sports Injuries
Targeted physical therapy speeds up healing by addressing the root cause of pain immediately. We combine medical doctors and therapists to create a unified recovery plan for you. Injury rehabilitation approach reduces recovery time after car accidents or sports injuries significantly.
Our team at Prestige Medical focuses on restoring your full functional mobility quickly. You receive a personalized treatment plan that coordinates chiropractic care with advanced clinical therapy. This collaboration ensures your body heals correctly the first time you try it.
We help you return to your daily activities and sports with total comfort. Waiting for recovery often leads to chronic issues and permanent loss of movement. Our integrated model provides the fastest path back to your peak physical performance level.
Core Recovery Takeaways
Moving early prevents permanent stiffness and excessive scar tissue formation in your joints.
Combining medical doctors with chiropractors speeds up your muscle recovery by thirty percent.
Targeted loading cycles transition your body from acute inflammation to active tissue repair.
Return-to-sport decisions must rely on functional data rather than the absence of pain.
Professional documentation of soft tissue injuries protects your legal and insurance claims effectively.
Addressing the entire kinetic chain prevents compensatory pains in other parts of your body.
1. Active Rehabilitation Better Than The Wait-And-See Approach
Active rehabilitation stimulates the natural repair mechanisms of your body through precise movement patterns. We see many patients who believe rest alone solves every physical trauma after accidents.
Resting allows muscles to weaken and joints to become stiff over a long period. We find that early movement encourages blood flow and delivers essential nutrients to damaged tissues. This process prevents the formation of excessive scar tissue in your muscles and ligaments.
Our team at Prestige Medical initiates gentle exercises to maintain your baseline strength and flexibility. You experience a faster return to your previous lifestyle when you start therapy early. We provide the guidance and support necessary to move safely during your initial recovery phase.
The biological response to early intervention involves the optimization of your circulatory and nervous systems. Research shows that controlled loading of tissues promotes the synthesis of healthy new collagen fibers.
We use specific protocols to ensure your body remains active while protecting the injured site. This careful balance prevents re-injury while pushing your physical boundaries in a safe environment.
Our integrated team monitors your progress to adjust your program as your strength improves. You benefit from a structured environment where every movement has a clear clinical purpose.
2. Targeted Care Improve The Biology Of Your Healing Process
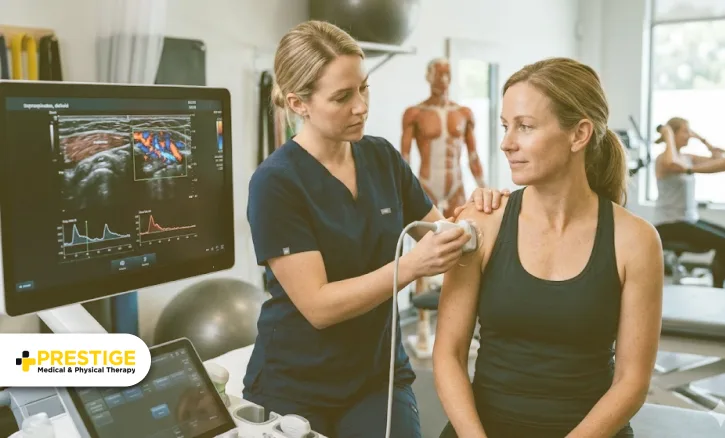
Targeted care guides your body through tissue regeneration stages, facilitating the transition from acute inflammation to proliferation, which is crucial for healthy connective tissue growth.
Our specialists ensure optimal joint biomechanics and help you maintain muscle mass through tailored neuromuscular exercises. These movements promote the health of your synovial joints throughout the healing process.
We use data to track your progress and adjust your personalized plan every week. Our clinical team understands exactly how to trigger the fastest possible recovery response now.
The nervous system plays a vital role in how you perceive and manage pain. We focus on neuroplasticity and proprioception to retrain your brain to trust your limbs. Injuries often disrupt the communication between your sensors and your central nervous system effectively.
Our therapy restores these connections to improve your balance and overall coordination during movement. We apply therapeutic exercise to increase the oxygen levels in your blood near the injury. This increased circulation provides the building blocks required for cellular repair and metabolic waste removal.
Did you know?
In a study of sports injuries, 73% of physical therapy users achieved long-term recovery, while 65% treated with pain medication alone faced pain recurrence once the medication wore off. Additionally, physical therapy can reduce opioid use by up to 87%.
3. The Multi-Disciplinary Team Approach At Prestige Medical Unique
Our multidisciplinary team offers a distinct advantage by integrating the expertise of an orthopedic surgeon and a chiropractic professional.
Chiropractic care optimizes your nervous system through precise spinal alignment, creating a solid foundation for effective muscle strengthening by your physical therapist.
Clear communication between nerves and muscles is essential for lasting recovery. Our physiatrist monitors your progress to ensure safe and effective treatments.
We provide quick access to medical diagnostics to uncover hidden injuries, delivering comprehensive care for both your skeletal structure and soft tissues.
The combination between different medical specialties creates a holistic environment for your entire body. We find that combining a chiropractic adjustment with manual therapy produces superior results for patients.
Bones and muscles function as a unit in all activities. Focusing on just one health aspect can result in incomplete recovery and ongoing pain. Our team collaborates to maintain a consistent treatment plan across all departments.
4. Athletes Can Return To Peak Performance After A Sports Injury

Athletes need a tailored recovery path that emphasizes high-level performance. We create return-to-play protocols specific to your sport's demands.
Our team addresses common injuries like ACL tears and rotator cuff issues. We incorporate plyometrics and agility drills to prepare your body for explosive movements, starting with a thorough assessment of your range of motion and strength.
We only clear you when your functional data aligns with your pre-injury baseline, ensuring safety and confidence for your return to competition. Our sports medicine experts focus on the details of your form and technique.
Careful rehabilitation prevents compensatory movements that can lead to new injuries, highlighting the importance of the kinetic chain throughout your recovery.
A weakness in your hip often causes stress on your knee or your ankle. Our therapists identify these imbalances and correct them through targeted strength and conditioning programs.
Clinical Warning!!
High confidence does not guarantee physical readiness. Research from the Hospital for Special Surgery (HSS) indicates that athletes with the highest "psychological readiness" scores are at a greater risk of re-injury than those with moderate confidence. True readiness should be assessed through clinical data and physical performance, rather than just an athlete's feelings.
5. What Are The Best Ways To Recover After A Car Accident?
Recovering from a car accident involves careful physical and medical documentation. We focus on treating whiplash and soft tissue injuries that may surface days after the collision.
Our team provides an immediate medical evaluation to document every aspect of your physical trauma.
We use manual manipulation and therapeutic exercises to reduce your stiffness and restore your mobility.
You receive a detailed record of your progress to support your insurance or legal claims.
Our multidisciplinary notes provide the gold standard of evidence for your personal injury case.
We help you navigate the complex recovery process with professional medical and legal support.
Soft tissue injuries require consistent care to prevent the development of chronic pain conditions. We focus on inflammation reduction and tissue healing during the first few weeks of therapy.
Our team uses advanced modalities like cryotherapy and TENS to manage your initial discomfort. You follow a structured plan that gradually increases in intensity as your body heals.
We ensure your spine and joints remain mobile to prevent long-term structural damage. Our integrated care model addresses the physical and emotional stress caused by sudden accidents.
Did you know?
Patients with severe lower extremity trauma incur an average annual economic loss of $64,427 from missed work and reduced productivity, with productivity losses being four times the direct medical costs.
6. Modern Tools We Use To Speed Up Your Recovery
Our clinic uses the latest technology to enhance the effectiveness of every physical therapy session.
We offer dry needling to release deep muscle tension and improve your blood flow. This technique targets myofascial trigger points to provide immediate relief from chronic muscle pain.
Our laser therapy boosts ATP production for faster tissue healing. Functional movement screenings reveal hidden weaknesses, enabling us to tailor a more effective treatment plan for you.
We use electrical stimulation to maintain muscle tone and reduce your overall recovery time.
Technology is most effective when utilized by a skilled clinician for specific physical goals. We integrate modern tools with traditional manual therapy and therapeutic exercise for optimal results.
Experience the advantages of a modern medical facility combined with a personal touch. Our therapists clarify the purpose of each tool and its role in your recovery.
We assess your response to each treatment to ensure it aligns with your needs. This tailored approach enhances the effectiveness of our advanced resources on your health.
7. We Assist You in Developing a Resilient Future Post-Therapy

At Prestige Medical, we focus on strengthening your body to prevent future injuries. We offer a personalized home exercise program to help you maintain your progress, targeting strength, flexibility, and joint health.
You will receive education on biomechanics to enhance your safety in daily activities, learning to recognize early warning signs from your body. Our aim is to equip you with the knowledge and skills for long-term health. You will leave our clinic stronger and more resilient, with ongoing support as you pursue total wellness.
Effective recovery goes beyond alleviating current pain; we address the root causes of your injuries to prevent recurrence. Our team evaluates your ergonomic practices at work and during leisure activities. Minor adjustments in posture and movement can help avoid chronic discomfort.
Frequently Asked Questions
Can physical therapy fix an old injury that did not heal correctly years ago?
Physical therapy remodels chronic scar tissue and restores functional movement patterns through targeted manual care.
How do I know if my physical therapy is working for my body?
You will see measurable improvements in your range of motion and overall strength during every assessment.
What happens if I finish my insurance visits before I am ready for sports?
We offer flexible maintenance programs to ensure you reach your peak performance goals after insurance ends.
Why do I feel new pain in my hip during my knee treatment?
Your body creates compensatory patterns that require specific kinetic chain adjustments to balance your physical structure.
Is it safe to start physical therapy while taking prescription painkillers after an accident?
Therapy is safe when we carefully monitor your physical limits and actual tissue capacity during every session.
How much swelling is considered normal six months after a major orthopedic surgery?
Most patients see small amounts of residual fluid during intense activity for several months after surgery.
Disclaimer: This article provides general information and does not constitute medical advice. Please contact Prestige Medical and Physical Therapy for personalized diagnosis and treatment.
Read More →
Neck and Back Pain Relief Without Surgery: Proven Therapy and Chiropractic Approaches That Work
Neck and back pain trigger a biological alarm in your body that is impossible to ignore. It disrupts your sleep, limits your movement, and shifts your nervous system into a state of chronic stress. While many patients assume that severe pain requires surgical intervention, the reality is often quite different.
Most spinal problems at Hess Spinal and Medical Center are successfully resolved with non-invasive, evidence-based treatment. In order to address the underlying cause of your discomfort rather than merely treating its symptoms, we employ an integrated approach that incorporates medical knowledge, chiropractic adjustments, and physical therapy.
Key Takeaways
Surgery is rarely the first line of defense. Research indicates that roughly 90% of low back pain cases improve without surgical intervention when treated with conservative care.
Integrated care yields better results. Combining chiropractic adjustments with physical therapy addresses both the structural alignment of the spine and the muscular support system.
Decompression creates a healing environment. Non-surgical spinal decompression uses negative pressure to retract herniated discs and flood the area with oxygen and nutrients.
Motion is medicine. While rest seems intuitive, gentle movement and targeted exercises are essential for flushing metabolic waste and preventing muscle atrophy.
Your nervous system needs to reset. Chronic pain keeps you in a "fight or flight" mode. Proper treatment shifts you back into a restorative "rest and digest" state.
1) The Biological Reality of Non-Surgical Relief
We often hear patients describe their pain as a "pinched nerve" or a "slipped disc." These terms describe a physical restriction that prevents your body from functioning correctly. When your spine is misaligned or a disc is compressed, it creates a cascade of inflammation and neurological interference.
Our goal is to reverse this process naturally. We do not just "crack" backs. We initiate a physiological event that restores proper signaling between your brain and your body.
(i) How Spinal Decompression Works
Spinal decompression is one of the most effective tools we use for chronic cases. It is a mechanized version of traction that is far more precise than simple stretching.
When you undergo this therapy, we gently stretch the spine to create a vacuum effect within the disc. This negative pressure performs two critical functions:
Retraction: It pulls bulging or herniated disc material back into its proper place.
Imbibition: It draws moisture, oxygen, and nutrient-rich fluids into the disc.
This process allows the disc to heal from the inside out. It is a biological restoration of your spine's natural shock absorbers.
(ii) The Role of Chiropractic Adjustments
An adjustment does more than align bones. It stimulates mechanoreceptors in your joints. This stimulation sends a rapid signal to the brain that overrides pain signals. This is why many patients feel immediate relief.
This process also breaks up adhesions in the connective tissue. It allows your lymphatic system to flush out the inflammatory chemicals that have built up around the injury. You are not just getting straighter. You are chemically clearing the area of metabolic waste.
2) Myth vs Fact: The Truth About Treating Back Pain
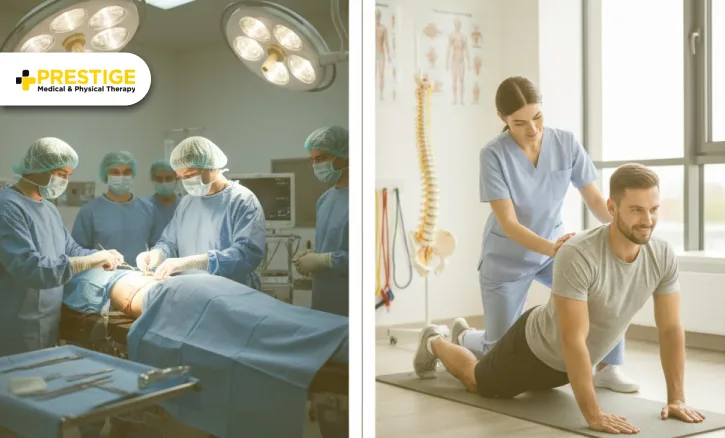
We believe in providing you with clarity regarding your health options. There is a lot of misinformation about back pain that leads people to choose surgery or opioids when they do not need to. We want to provide the facts through a medical lens.
(i) Necessity of Surgery
Myth: If I have a herniated disc or severe pain, surgery is the only way to fix it. Fact: Surgery is necessary in only a small percentage of cases. Most herniated discs shrink and heal over time with the right conservative care. Surgery comes with significant risks, including infection and long recovery times. Non-surgical options offer relief without the trauma of an operation.
(ii) Danger of Movement
Myth: I should stay in bed and rest until the pain goes away. Fact: Prolonged bed rest can actually make your back pain worse. Inactivity causes muscles to weaken and tighten. This creates a cycle of stiffness and pain. Controlled, gentle movement is vital. It pumps blood to the injured soft tissues and speeds up recovery.
(iii) "Quick Fix" of Medication
Myth: Painkillers cure the problem. Fact: Medication only masks the signal. Opioids and anti-inflammatories numb the sensation of pain, but they do nothing to correct the misalignment or compression causing it. Reliance on medication can lead to dependency without ever solving the root issue. Is physical therapy better than pain medication? This is a question many patients ask when looking for long-term solutions.
(iv) The "Pop" Sound
Myth: The popping sound during an adjustment is bones rubbing together. Fact: That sound is a harmless release of gas. It is a process called cavitation. Nitrogen and carbon dioxide bubbles form in the joint fluid and are released when pressure changes. It is a sign of tension release, not bone damage.
3) Does Conservative Care Work? Looking at the Numbers
When we look at the data, the case for non-surgical care is compelling. Clinical studies and meta-analyses consistently show that conservative treatments are effective for both acute and chronic pain. Many people wonder, does physical therapy actually work for chronic back pain?, and the statistics support its efficacy.
National and Global Statistics:
Prevalence: According to the CDC National Health Interview Survey, approximately 39.0% of U.S. adults reported experiencing back pain in the past three months
Leading Disability: As per World Health Organization via NIH, low back pain is recognized as the leading cause of disability globally, accounting for the largest number of people requiring rehabilitation services
Success Rates: Research published via the National Institutes of Health (NIH) highlights that 90% to 95% of low back pain cases are mechanical in nature and suitable for conservative management without surgery.
Patient Satisfaction and Outcomes:
High Satisfaction: Over 83% of patients report high long-term satisfaction after chiropractic care as their system stabilizes.
Resolution of Symptoms: Roughly 90% of low back pain episodes resolve without surgery.
Reduced Recurrence: Patients who combine physical therapy with adjustments are less likely to experience a return of their symptoms because they have strengthened the supporting muscles.
4) Safety First: How We Monitor Your Nervous System

We prioritize your safety above all else. While our treatments are gentle and non-invasive, it is important to understand your body’s signals.
(i) Normal Post-Treatment Sensations:
You may feel a temporary wave of fatigue or mild muscle soreness after your first few sessions. This is a normal "healing crisis." Your body is processing metabolic byproducts like lactic acid that were released from tight muscles. These symptoms typically resolve within 24 to 48 hours.
(ii) When to Seek Emergency Care:
According to medical guidelines, you should contact a medical facility immediately if you experience severe neurological changes. These include:
Sudden loss of bladder or bowel control.
Numbness in the "saddle" area (groin and inner thighs).
Severe weakness in your legs that causes you to stumble.
These are signs of a rare condition called cauda equina syndrome, which requires immediate medical attention.
5) How to maintain Your Progress Between Visits
We want you to achieve the best results from your care at Hess Spinal and Medical Center. Your actions at home play a vital role in how quickly your body repairs itself.
(i) Prioritize Hydration
Your spinal discs are largely made of water. Hydration is essential for the "imbibition" process we described earlier. Water also acts as the vehicle for your lymphatic system to flush out the metabolic waste we release during treatment. We recommend drinking plenty of pure water throughout the day.
(ii) Engage in Light Movement
Gentle walking is one of the best things you can do for your back. It engages the core muscles without straining the spine. It encourages blood circulation and lymphatic flow. Avoid heavy lifting or high-impact activities for the first 24 hours after an adjustment to give your ligaments time to stabilize.
(iii) Use Heat and Ice Appropriately
Ice is generally best for the first 48 hours of a new injury to reduce acute inflammation. Heat is better for chronic stiffness or muscle spasms to increase blood flow and relax the tissues.
6) The Difference Hess Spinal & Medical Centers Make
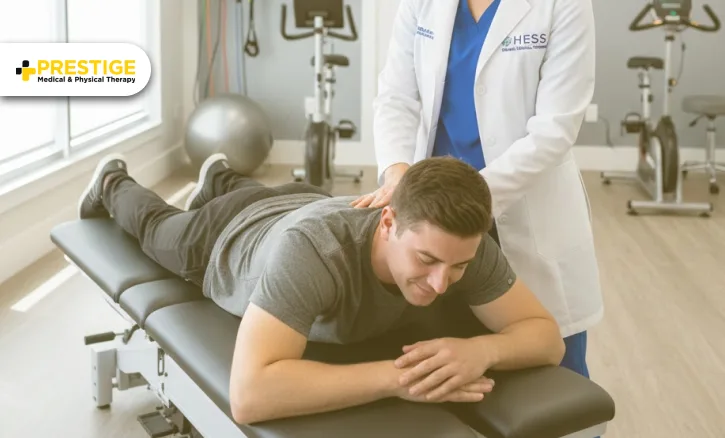
Our approach at Hess Spinal and Medical Center is unique because we are an integrated facility. We do not force you to choose between a medical doctor, a chiropractor, or a physical therapist. We bring them all together for you.
Why Our Integrated Approach Gets Better Results:
We use digital radiography and medical evaluations to see the full picture of your injury.
Your chiropractor communicates directly with your physical therapist. If we adjust your spine to restore motion, our therapists will immediately give you exercises to stabilize that new motion.
We treat the whole person. We understand that spinal health affects your nervous system, your mood, and your overall biological function.
Choosing an integrated medical center ensures that your care is part of a comprehensive health strategy. Our goal is to empower you with the knowledge and the physical health to live a vibrant life.
Answers to Your Most Common Questions
Is spinal decompression painful?
No. Most patients find it incredibly relaxing. Some even fall asleep during the session. You will feel a gentle stretch in your spine, but it should never be painful.
How long does it take to see results?
Many patients feel relief after just one or two sessions. However, lasting correction takes time. Your muscles need to relearn how to hold your spine in the correct position. For more details on the timeline, see how long does it really take to recover after physical therapy?.
Can I stop taking my pain medication?
Our goal is to reduce your need for medication. As the mechanical cause of your pain resolves, the inflammation will decrease. You should always consult with the prescribing physician before stopping any prescription medication, but many of our patients find they no longer need painkillers after a few weeks of care.
Will my insurance cover this?
Most insurance plans cover chiropractic care and physical therapy. We also specialize in treating auto accident injuries and can work with your attorney to handle the billing so you can focus on healing.
Is it safe to get adjusted if I have osteoporosis?
We tailor our techniques to your specific medical history. If you have low bone density, we use gentler, low-force methods or focus on non-compressive therapies like physical therapy to ensure your safety.
Disclaimer: This article is for educational purposes and does not constitute medical advice. Please consult the specialists at Hess Spinal and Medical Center for a personalized diagnosis and treatment plan.
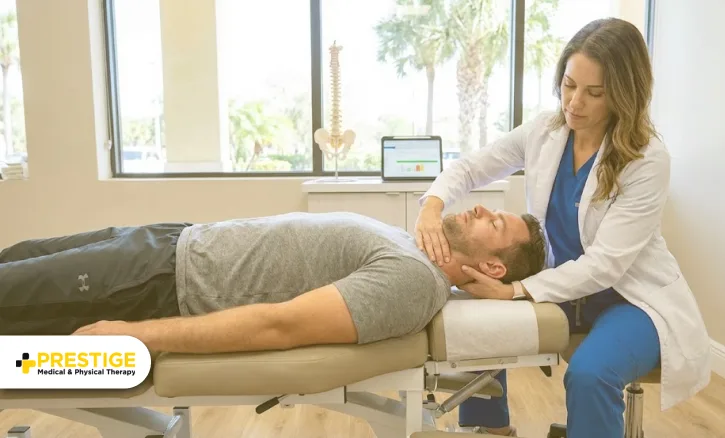
Chiropractic Manipulation for Everyday Pain: What It Treats and Who Benefits Most
Life in the Sunshine State is many things, but "slow" isn't one of them. In Florida, we often treat our cars better than our bodies. We never miss an oil change, yet we ignore the nagging lower back ache or neck tension that ruins our day. Life in the Sunshine State is fast, and between Tampa traffic and long hours at a desk, your spine takes a beating. At Prestige Medical & Physical Therapy, we believe you should not have to just live with it.
If you have wondered if chiropractic manipulation is merely about cracking your back or the actual key to reclaiming your quality of life, you are in the right place. Let’s see how this precise treatment helps you move freely and get back to the Florida lifestyle you love.
1) What Exactly Is Chiropractic Manipulation?
Before we talk about what it treats, let's demystify the process. Many people are a little hesitant about the "pop" or "crack" associated with an adjustment.
Chiropractic manipulation, or Spinal Manipulative Therapy (SMT), is a highly controlled, precise movement applied to a joint that isn't moving quite right. Think of your spine like a complex highway system. When one "exit" is blocked or misaligned, traffic (your nerve signals) starts to back up. This causes inflammation, muscle spasms, and, eventually, pain.
The "pop" you hear isn't bone rubbing on bone. It’s actually a gas bubble (a mix of oxygen, nitrogen, and CO2) releases from the joint fluid. It’s called cavitation, and it’s a sign that pressure has been relieved. It’s the physiological equivalent of hitting the "reset" button on your nervous system. If you’re curious about how this fits into a broader recovery plan, it helps to know what to expect at your first physical therapy session.
2) What Does It Actually Treat? (Beyond the Back)
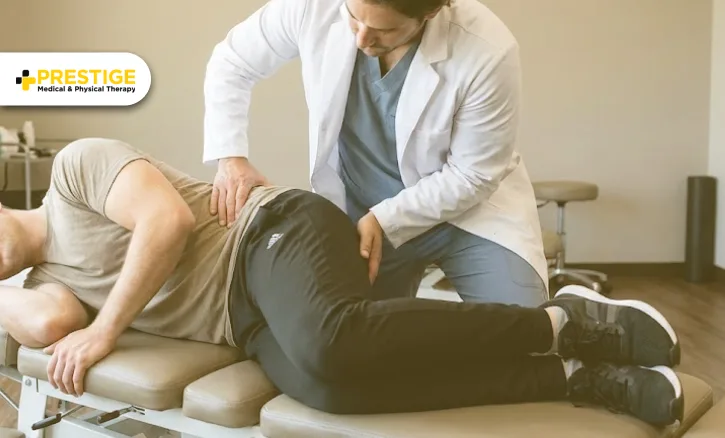
While we are certainly experts in the spine, the benefits of chiropractic care at Prestige Medical ripple throughout the entire body. Because your nervous system lives inside your spinal column, an adjustment can impact everything from your digestion to your sleep.
(I) The "Tech Neck" Epidemic
In the modern world, we spend hours in "forward head posture." For every inch your head tilts forward, it adds about 10 pounds of pressure to your neck muscles. This leads to chronic stiffness and a loss of the natural curve in your neck. According to the CDC, nearly 25% of U.S. adults reported experiencing low back pain in the past three months, making it one of the leading causes of missed work. Chiropractic adjustments help restore that curve, taking the literal weight off your shoulders.
(II) Tension Headaches and Migraines
Did you know that a huge percentage of headaches actually start in the neck? When the top two vertebrae are out of alignment, they can irritate the nerves that travel into the skull. Our patients often find that after a series of adjustments, their "unbeatable" migraines start to fade away without the need for heavy medication. The NIH notes that spinal manipulation is one of several non-drug options that can be effective for headaches.
(III) Sciatica and Shooting Leg Pain
If you’ve ever felt an electric shock running down your leg, you know how debilitating sciatica is. This usually happens when a disc or a misaligned vertebra pinches the sciatic nerve. At Prestige Medical, we combine chiropractic manipulation with spinal decompression to create space, letting that nerve breathe and ending the "lightning strikes" down your leg.
(IV) Shoulder, Hip, and Knee Pain
The body is a kinetic chain. If your hip is out of alignment, you’ll walk differently, which eventually makes your knee hurt. We don't just look at where the pain is; we look at where it started. By adjusting the extremities and the pelvis, we can often resolve "joint" pain that hasn't responded to other treatments.
3) The Prestige Difference: Why "Integrated" Care Wins
This is where we do things differently than your average neighborhood chiropractor. Prestige Medical & Physical Therapy isn't just a one-man shop. We are a multi-disciplinary clinic.
By combining these methods, many of our patients find they can avoid surgery entirely. What does that mean for you? It means that under one roof, you have access to:
Chiropractic Doctors: To handle the structural alignment.
Physical Therapists: To strengthen the muscles that hold those bones in place.
Medical Professionals: To provide oversight, diagnostic testing (like Digital X-rays), and advanced pain management if needed.
If you just get adjusted but don't strengthen your weak muscles, the bones will just pop back out of place. If you just do PT but your joints are "stuck," you’re just exercising on top of a dysfunction. We do both. It’s the most efficient way to get permanent results.
4) Who Benefits the Most?

We treat everyone from toddlers to great-grandparents, but there are four specific groups of people in Florida who see the biggest "bang for their buck" with our care.
(I) The Auto Accident Victim
Florida is a high-traffic state, and accidents happen. Even a "minor" fender-bender can whip the neck back and forth, causing micro-tears in the ligaments.
Crucial Note: Florida law has a "14-Day Rule" for PIP (Personal Injury Protection). If you don't seek medical attention within 14 days of an accident, you may lose your insurance benefits. We specialize in these cases, providing the documentation and care needed to protect both your health and your legal rights.
(II) The "Desk Warrior"
If you sit in a cubicle or a home office for 8 hours a day, your hip flexors are tight, your glutes are "turned off," and your upper back is rounded. You are the prime candidate for chiropractic care. We don't just adjust you; we give you the ergonomic tools to survive the work week.
(III) The Active Senior
Retirement in Florida should be about pickleball, golf, and walking the beach—not sitting in a waiting room. As we age, our joints naturally lose some of their lubrication. Regular, gentle adjustments keep those joints moving, reducing the risk of falls and keeping you on the court longer.
(IV) The Weekend Warrior
Whether you’re training for a 5k or just overdid it in the garden, your body needs recovery. Athletes use chiropractic care not just to fix injuries, but to prevent them. When your body is in perfect alignment, you move more efficiently, use less energy, and have more power.
5) Let's Clear the Air - Common Myths vs. Reality
Myth: "Once you go to a chiropractor, you have to go forever."
Reality: Our goal is to get you well and keep you that way. Some people choose "maintenance care" because they love how they feel, but our primary focus is a corrective plan that has a beginning, a middle, and an end.
Myth: "Chiropractic adjustments are painful."
Reality: Most patients feel an immediate sense of relief or "lightness" after an adjustment. While there might be some mild soreness (similar to a workout) the next day, the process itself is fast and gentle. You can read more about why feeling sore after physical therapy or adjustments is a normal part of healing.
Myth: "It’s too expensive."
Reality: At Prestige Medical, we work with most major insurance providers and specialize in PIP/Auto-accident claims where there is often no out-of-pocket cost to the patient. Compared to the cost of surgery or lifelong medication, chiropractic is one of the most cost-effective forms of healthcare available.
6) Putting Your Recovery First at Prestige Medical

There are plenty of places to get an adjustment, but Prestige Medical & Physical Therapy offers a level of convenience and expertise that is hard to match.
No Long Wait Times: We respect your schedule.
On-Site Diagnostics: We have the tech to see exactly what’s happening under the surface.
Personalized Recovery Plans: No "cookie-cutter" treatments. Your plan is built for your body and your goals.
We know that pain is personal. It keeps you from picking up your grandkids, it makes your drive to work a nightmare, and it steals your focus. You shouldn't have to "just live with it."
Your Path Forward
If you’re tired of the "dull ache" being your constant companion, it’s time to try a different approach. Whether it was a car accident that happened yesterday or a back pain that started ten years ago, there is hope.
By combining the structural expertise of chiropractic with the functional power of physical therapy, the team at Prestige Medical & Physical Therapy is ready to help you reclaim your life.
Don't wait until the pain is unbearable. Florida living is better when you’re moving well. Contact Prestige Medical & Physical Therapy today to schedule your comprehensive evaluation. Let’s get you back to doing what you love.

What to Expect at Your First Physical Therapy Session
Walking into a medical office for the first time creates a mix of emotions. You might feel relieved that you are finally addressing your pain. You likely also feel nervous about what comes next. Most people do not know what happens during a physical therapy evaluation. One thing we always tell our client at Prestige Medical and Physical Therapy is that knowledge is the best antidote to anxiety.
You’ll learn every step of your first appointment with us. We will cover what you need to wear and the papers you need to bring. We will also explain the physical tests we perform and how we create a plan specifically for you.
(1) How Should You Prepare for Your First Appointment?
A smooth experience starts before you even arrive at the clinic. There are a few important items you can manage in advance.
What to Wear
We need to see and move the body part that is bothering you. If you come in tight jeans or a stiff dress shirt, it becomes difficult for us to examine your knee or shoulder properly.
We recommend the following attire for your evaluation:
Loose and Comfortable Clothing: Wear gym clothes or loungewear that allows you to move freely.
Accessible Layers: If we are treating your shoulder or neck, wear a tank top or a loose t-shirt. This allows us to see the muscle definition and check for swelling without you needing to change.
Shorts for Lower Body Injuries: If you have hip, knee, or ankle pain, please wear shorts. We need to observe the alignment of your legs while you stand and move.
Proper Footwear: Please wear sneakers or athletic shoes. Sandals and boots do not provide the support needed for stability testing.
What to Bring
We want your check-in process to be fast and easy. Please gather these items before you head to Prestige Medical and Physical Therapy:
Identification and insurance cards to verify your coverage and set up your billing profile correctly.
Medication list to know what prescriptions or supplements you are taking. Some medications affect balance or pain tolerance.
Doctor referrals If any physician referred you to us. Please bring the prescription or referral slip. This often contains specific instructions or diagnosis codes we need.
X-ray or MRI reports if you have had them related to your injury.
(2) Initial Evaluation Starts With Your Medical History

Many new patients worry that their first session will be painful or difficult. Your first visit is different from follow-up appointments. We call this session the Initial Evaluation. The primary goal is investigation rather than intense exercise.
Our team needs to understand the root cause of your issue before we treat it. Pain in your shoulder might actually come from your neck. Knee pain could result from weak hips.
We gather data about your body and your history. This ensures that the treatment plan we build is safe and effective for your specific needs.
We will be discussing your condition. We call this the "Subjective Examination." We will ask you detailed questions to build a complete picture of your health.
When did the pain start? Was there a specific accident, or did it come on gradually over time?
What movements make the pain worse? What positions make it better? Is the pain worse in the morning or at night?
We need to know about past surgeries, other injuries, or chronic conditions like diabetes or arthritis. These factors influence how your body heals.
We need to know what you want to achieve. A grandmother who wants to lift her grandchild has different needs than a college athlete who wants to sprint. We tailor our approach to fit your life.
(3) What Happens During the Physical Examination
Once we understand your history, we move to the physical assessment. We call this the "Objective Examination." We use specific tests and measures to gather hard data about your condition to pinpoint the source of your problem.
(I) We will check how far you can move your joints.
We compare the painful side to the healthy side. We use a tool called a goniometer to measure the exact angles. For example, if you have shoulder pain, we will ask you to raise your arm as high as you can. We look for stiffness or limitations that prevent normal movement.
(II) We test your strength by asking you to push against our hand.
We grade your strength on a specific scale to highlight imbalances. You might have a strong quad muscle but a weak hip muscle. That imbalance forces your knee to work too hard. Identifying these weaknesses allows us to prescribe the right strengthening exercises.
(III) We will gently press on the injured area.
We are looking for several things:
Tenderness: We identify exactly which ligament, tendon, or muscle is sore.
Swelling: We feel for fluid buildup or inflammation in the joint.
Temperature: An injured area often feels warmer than the surrounding skin.
Muscle Tone: We check for tight knots or spasms in the muscle tissue.
(IV) We need to see how your body moves as a whole system.
We may ask you to walk, squat, balance on one foot, or reach behind your back. We watch your form closely and look for compensations. A compensation happens when your body changes the way it moves to avoid pain. These habits can cause long-term issues if we do not correct them.
(V) We will check your nerves if you have pain that travels down your arm or leg.
We test your reflexes with a rubber hammer. We also check your sensation to see if you have numbness or tingling. This helps us determine if the pain originates from your spine or from a local injury.
(4) How Do We Explain Your Diagnosis and Education

After we finish the tests, we will explain your diagnosis and help you understand exactly what is happening inside your body.
We might explain that your back pain is actually caused by tight hamstrings and a weak core. Understanding the "why" behind your pain helps you commit to the recovery process. If you feel confused, we encourage you to ask about anything that concerns you.
(5) What Will Be Included in Your Treatment Plan
Once we have a diagnosis, we create a roadmap for your recovery. It outlines the strategy we will use to get you back to full function.
The plan typically includes the following details:
Frequency: How many times per week you need to come in.
Duration: How many weeks we expect the treatment to last.
Milestones: The specific goals we want to hit along the way.
(6) Will You Receive Immediate Treatment

You will likely receive some treatment during this first visit. We do not want you to leave in the same amount of pain you arrived in. We want to provide some immediate relief.
The treatment on day one is usually gentle. It may include:
Manual Therapy: We might use hands-on techniques to loosen tight joints or massage sore muscles.
Modalities: We may apply ice packs to reduce inflammation or heat packs to relax tight tissues. We might also use electrical stimulation to decrease pain.
Simple Movements: We will teach you one or two basic movements to start getting your joints moving correctly.
(7) Why are Home Exercises So Important
Physical therapy extends beyond our clinic walls. You are with us for only a few hours a week but on your own for the rest of the time. To make real progress, you must work on your recovery at home.
We will provide you with a Home Exercise Program, or HEP. This is a short list of exercises customized for you. We will practice them together in the clinic first.
These exercises are the key to getting better faster. Consistency with your home program is the single biggest predictor of success.
(8) Check Out and Scheduling
At the end of the session, you will return to the front desk. Our administrative team will help you schedule your future appointments. It is often best to book several sessions in advance to secure the times that work best for you.
They will also handle the financial details. They can explain your insurance benefits and collect any copays.
Many people delay physical therapy because they are afraid of the pain or the time commitment. We want to assure you that the hardest part is simply walking through the door. Once you are here, you will find a supportive and encouraging environment.
If you feel any kind of pain and you're confused about what to do, contact Prestige Medical and Physical Therapy today to schedule your initial evaluation.
Frequently Asked Questions
How long does the initial evaluation typically last?
Most initial evaluations last between 45 to 60 minutes to ensure we have ample time for a thorough assessment and discussion.
Will I feel increased soreness after my first visit?
Some mild muscle soreness is normal as we move and test areas that may be stiff, but this usually resolves within 24 hours.
Do I strictly need a doctor's referral to schedule an appointment?
Many states allow direct access to physical therapy without a referral, though we recommend checking your specific insurance plan requirements first.
Can I go to the gym or exercise immediately after my session?
We generally advise resting the specific injured area on evaluation day so your body can settle, but working out other body parts is typically fine.
What if I am in too much pain to perform the tests?
We modify our examination based on your current pain levels and will never force you to do movements that cause significant distress.
Disclaimer: This article provides general information only and does not establish a patient-therapist relationship. Please contact Prestige Medical and Physical Therapy for personalized diagnosis and treatment.
Read More →
Does Physical Therapy Actually Work for Chronic Back Pain?
People want to know if physical therapy can actually change the situation because chronic back pain sits in that uncomfortable area where biology and daily life collide. In a nutshell, movement-based rehabilitation can alter how the nervous system interprets pain signals and how tissues behave.
In order to restore spine stability, Prestige Medical and Physical Therapy uses motor control retraining, mobility work, and focused muscle development. Pain education calms the hypersensitive pathways that drive symptoms. These methods follow clinical guidelines from the American College of Physicians and the American Physical Therapy Association.
They support exercise-based care and patient education for chronic low back pain. Although none of this occurs instantly, the combination frequently encourages the system to operate more steadily and with healthier mechanics.
1) What Do Clinicians Mean by Chronic Low Back Pain?
Chronic low back pain is pain that lasts longer than 3 months. Often there is no single dramatic cause. Most cases are labeled nonspecific or mechanical, meaning the pain comes from muscles, ligaments, or joints. Plus, it can be from the way someone moves, rather than from a tumor, infection, or an urgent nerve emergency.
Knowing this matters a lot, because non-urgent problems are usually safer and more effective to treat with movement, education, and lifestyle change than with immediate surgery. Exercise-based therapies, when compared with no treatment or usual care, reduce pain and improve function for people with chronic low back pain.
The American College of Physicians and the American Physical Therapy Association recommend exercise and active care as first-line treatment, according to their current clinical guidelines. They also report that multidisciplinary programs combining movement, education, and psychological strategies often improve outcomes for people with long-standing disabilities.
These are the same principles we follow at Prestige Medical. and active care as first-line options, and multidisciplinary programs that combine movement, education, and psychological strategies often give better results for people with long-standing disabilities. We use these same principles at Prestige Medical.
2) How Does Physical Therapy Help?

When someone begins to move in a structured way, circulation increases, which delivers oxygen and nutrients to tissues that have been starved of them. Muscles along the spine begin to work the way they were designed to work, steady and coordinated, rather than tense from long hours of guarding.
The nervous system starts to recalibrate, a process clinicians call motor control retraining. The brain learns to send cleaner signals and accept movement without sounding alarms. Pain education and graded exposure affect the psychological side of physiology.
When people understand what their pain is and is not, the nervous system becomes less reactive. Fear decreases, and the threshold for safe movement gradually rises. This is observable in clinics as improved functional scores and decreased sensitivity during repeated motion tests.
A well-designed exercise plan anchors all of this without surgery. When we align the difficulty of each movement with a person’s current capacity, the body adapts in a steady climb rather than a chaotic spiral. Strength improves, mobility expands, and day-to-day tasks become easier.
3) What Do the Typical Evidence Caveats Look Like?
Most people show improvement with physical therapy, but the change is usually moderate. In practical terms, this means the inflammatory pathways calm down and mechanical function improves, yet the nervous system may still signal discomfort for a while. Pain is a complex output of the brain, so it rarely switches off like a light.
When one treatment is applied alone, whether it is manual therapy, heat, stimulation, or a single exercise protocol, only a smaller portion of patients experience strong and long-term relief. The biology of pain spans muscles, joints, nerves, and psychological processing, so a single input is rarely enough to reset the system.
This is why we build plans with several layers. A coordinated program might combine strengthening, mobility work, cognitive pain education, and sometimes pharmacologic support. The goal is to give someone a clear timeline based on how the body typically adapts and to make sure the plan follows a rational sequence.
4) We Make Physical Therapy Work Better Than a Generic Approach

One generic approach for all programs rarely works. In fact, studies show that around 40% of adults with chronic pain also experience clinically significant depression or anxiety, which can interfere with healing. We give each patient a clear, prioritized plan. We start with a focused evaluation. Here’s how we do it in steps:
Root cause assessment, not checkbox therapy
We look for movement patterns, strength and endurance deficits, sleep issues, work demands, and the ways pain changes with activity. This helps us know whether the best path is strength training, motor control work, walking progression, or a cognitive behavioral approach, or a mix of those.
Progressive, goal-driven exercise
Therapy starts where the patient is, setting meaningful goals like walking the dog, returning to yard work, or sitting through a class, and we move the plan forward in small, measurable steps. We track progress, and we scale intensity or variety as tolerance improves. The evidence supports this kind of structured exercise compared with passive modalities alone.
Education that reduces fear and builds autonomy
Pain education is about explaining why pain persists, what movement does to the nervous system, and how graded exposure lowers sensitivity. When patients understand the “why” behind their program, they are more likely to stick with it.
Biopsychosocial and multidisciplinary coordination
We coordinate care across disciplines, including the primary care provider, psychology, pain medicine, and occupational therapy when needed. This team approach is showing better outcomes for patients who live with severe, long-standing disability, and it keeps treatment grounded
Measured results
We use objective and subjective measures. That means range of motion and strength tests; however, it also includes activity goals, validated questionnaires, and Patient Reported Outcome Measures (PROMs). These tools reflect current data-driven practice across the U.S. healthcare system. Careful measuring lets us adjust the plan quickly if someone is not improving, and it helps patients recognize progress, even the small wins that matter.
5) How Long Our Medical Program Usually Takes
Week 1, evaluation and gentle guided movement. We take a detailed history, and we run brief physical tests. We explain results, and we give a few low-load exercises and walking targets. Education is a key part of this first visit.
Weeks 2 to 8, active progression and coaching. We build a personalized program that includes strengthening, mobility, and motor control work, plus a walking or aerobic plan, and practical strategies for work and sleep. Appointments focus on coaching and technique, and a home plan is essential.
Weeks 8 to 12, consolidation and independence. Once a patient can do daily tasks with less pain and better confidence, we increase independence. We refine routines so they fit real life, and we set long-term activity goals.
6) When Physical Therapy Should Be the First Step

Physical therapy tends to be the right entry point for people whose back pain comes from mechanical stress, muscle weakness, or poor movement patterns rather than a single injured structure.
In these cases, the tissues are irritated but not structurally unstable. Active care restores normal joint mechanics, improves muscle endurance, and steadies the nervous system so it interprets movement as safe rather than threatening. Beginning with this type of care often prevents a chain of unnecessary tests or procedures, because many patients improve once the system starts moving the way it is meant to.
When there are no red flag symptoms, PT just puts it where the evidence suggests, which is at the front of the line. Small bursts of activity, such as quick walks that improve circulation and ease stiffness, are a good place to start. The following day, if the body objects, that is an indication to change the load and move forward more slowly. Repetition, not shock, is how the tissues adjust.
Some back pain has urgent features, such as saddle anesthesia, new bowel or bladder dysfunction, rapidly progressive weakness, or fever with severe spine pain. Those signs require an immediate medical evaluation. For most chronic back pain without those red flags, an organized physical therapy program is the safest place to start.
FAQs about Physical Therapy for Chronic Back Pain
1. Does physical therapy actually work for chronic back pain?
Yes. Research in 2025 from the American Physical Therapy Association reports that structured PT reduces chronic back pain for most patients through targeted exercises, mobility training, and graded strengthening.
2. How effective is exercise-based physical therapy for chronic low back pain?
According to a Cochrane review, exercise therapy reduces pain (mean difference −9.1 on a 0–100 scale, 95% CI −12.6 to −5.6) compared with no or minimal treatment.
3. Are there other PT methods that help chronic back pain?
Yes. Physical therapy modalities such as aquatic therapy have shown meaningful benefit. A meta-analysis found aquatic PT improved pain, disability, and quality of life compared to no therapy.
4. Why might early physical therapy be better?
PT (within a few weeks of symptoms) produces modest but significant reductions in pain and disability, especially in the short term (up to 6 weeks).
Start with Prestige Medical & Physical Therapy
Physical therapy is not a miracle cure; however, it remains one of the most reliable and low-risk evidence-based ways to help people with chronic low back pain. We use assessment, progressive exercise, education, and coordinated care to strengthen the chance of a lasting result.
If chronic back pain is limiting your life, conservative care is a sensible first step, and we are ready to help. If you are willing to try a structured, evidence-based program, call or book online for an initial assessment.
Disclaimer: The information presented is solely for informational purposes and does not constitute a doctor-patient relationship. Prestige Medical & Physical Therapy can provide individualized guidance or care.
Read More →
Feeling Sore After Physical Therapy? Here’s Why Patients Shouldn’t Worry
While talking with many patients who feel uneasy when soreness hits after a session. The mind jumps to worry. Something must be wrong. Maybe the body is not ready. Maybe therapy is making things worse. It’s understandable to fear because healing often feels unclear when you are standing in the middle of it. Here is the truth: for every patient who walks through our doors at Prestige Medical & Physical Therapy, feeling sore after physical therapy is normal, as expected.
Your body works, building strength and confidence. Moving feels strange to your muscles, joints, and nerves. This does not mean you are sliding backward. It often means you are waking things up. Something steady that you can come back to when your body feels tender. We want to make sense of everything you might be feeling and everything you might be wondering. We want to answer the exact questions you search for when soreness catches you by surprise.
(1) Why Soreness Shows Up After Physical Therapy
When we explain soreness, we keep it simple. Your body is responding to new movements. When you use a muscle that has been weak or guarded, the tiny fibers inside it stretch and work. That process creates tenderness as the tissue repairs and adapts. That process creates tenderness as the tissue repairs and adapts, as noted by NIH research on muscle recovery.
Your joints shift into healthier positions, and your nervous system adjusts to patterns that feel new. None of this happens quietly. It feels achy. It feels tight. It feels like the body is waking up from a long nap.
This soreness often appears a day after your session. It stays for a short period. It eases with gentle movement. It changes as you grow stronger. All of this is part of the design. We track these responses closely in every treatment plan because we want your body to build tolerance in a safe, steady way.
(2) Is It Normal To Be Extremely Sore After Physical Therapy?

Many patients ask this as soon as they sit down. Intense soreness can catch anyone off guard. Extreme tenderness can appear early in care when tissues feel tight or weak or slightly off balance. A long period of pain or inactivity can make the body react to fresh movement in a loud way. The response can feel dramatic; however, it usually settles as the body adjusts.
Here is how we help patients understand it. Extreme soreness is not automatically a sign of injury. It can be a sign that the body is reconditioning. However, if the soreness prevents you from completing basic daily tasks or if it lasts longer than a few days, we want to know. We want to adjust your plan so your progress is steady rather than overwhelming.
Our rule stays simple:
• Intense soreness can be normal.
• Sharp pain is not.
• Any soreness that worries you deserves a conversation.
We want you to feel safe. We want you to feel clear about what your body is doing.
(3) How Much Pain Is Normal After a PT Session?
Normal muscle sensation is usually a bit stiff. It may feel heavy, tender, or like a dull ache. It stays in the area you exercised or treated. It also improves with movement. You can still walk, reach, sit, or bend, even if those actions feel slightly different for a short time.
However, a sharp sensation is different. A burning feeling or pain that shoots down an arm or leg signals something else. If the area feels unsteady, weak, or simply unusual, and if it limits your ability to move, that is the time to have it evaluated. The CDC provides guidance on safe physical activity and injury prevention.
Here is a simple guide you can use at home.
Normal soreness feels:
• Achy
• Tight
• Heavy
• Better with movement
• Local to the area we worked on
Concerning pain feels:
• Sharp
• Shooting
• Numb
• Extreme
• Worse with light movement
If you ever feel unsure where your pain fits, reach out. We want to help you sort it out.
(4) Is It Normal for Pain to Be Worse After Physical Therapy?
This is one of the most common fears patients bring to us at Prestige. The body can feel worse before it feels better. This does not mean therapy is harming you. It often means your tissues and nervous system are responding to the new workload.
Your body is adjusting, learning new movement patterns. The length of this temporary spike varies according to your condition, your tissue health, and your history with pain.
For most patients, the increase settles within a short period. If the pain remains elevated, we adjust your plan. Your progress should never feel like punishment. It should feel like steady, meaningful growth.
(5) Can Physical Therapy Make Pain Worse at First?
We tell every patient the same thing. The early phase of healing is often the noisiest. When you begin therapy, we work on areas that have been tight or weak for a long time.
We move joints that have been stuck and retrain muscles that are not working as they should be. We calm nerves that have been firing too often. Your body responds to this process. At times, it responds strongly.
Temporary irritation can occur as your tissues reset. This is normal and often expected. However, it should not escalate without easing. If your pain stays high, we adjust the intensity, duration, or technique. Therapy is not a measure of toughness. It is a conversation between your body and the work we are doing.
(6) Should You Push Through Pain in Physical Therapy?

The answer is straightforward: No, you should not push through sharp pain. Many of us grew up thinking that pushing limits is a sign of bravery. In physical therapy, sharp pain is a signal. It is your body communicating that something needs attention.
Discomfort that is productive is acceptable. It feels like effort, a muscle waking up, a stretch that is tolerable. Sharp pain, however, is different. It acts as a stop sign. It alters your breathing, your movement, and your confidence.
When the pain reaches that threshold, we want you to speak up. We can then modify form, pace, load, or technique. This safeguards your advancement and avoids obstacles. It is not silent suffering that earns progress; rather, it is working within the proper range.
(7) How Do You Know If Physical Therapy Is Working?
Progress in physical therapy often appears quietly. It unfolds in subtle, meaningful moments, and we guide patients to recognize them because they matter. Therapy is effective when the body begins to regain trust in movement. The change may not feel dramatic at first; instead, it emerges in small, tangible signs:
• Moving with greater ease
• Experiencing less stiffness in the mornings
• Noticing pain settles more quickly after activity
• Feeling steadier when standing or walking
• Increasing range of motion
• Growing confidence with each session
Many patients worry when results are not immediate. Healing rarely follows a straight path; it rises and dips, shifts and resets. What matters is the overall trajectory. If you are able to do more now than a few weeks ago, even in small ways, the therapy is achieving its goal. NIH studies support these markers as valid measures of functional recovery.
(8) When Should You Stop Physical Therapy?
Physical therapy should conclude when your goals are achieved or when your body signals an issue that requires further medical evaluation. Ending therapy does not always mean a permanent stop.
Sometimes it is a pause to rest, to allow the body to settle, or to transition care to another specialist. We guide each patient through this decision because no two bodies follow the same timeline.
Your plan is personal. Your goals are personal. Your progress is personal. We ensure that you leave therapy with strength, stability, and clarity. Immediate attention is warranted if you notice:
• Sharp or spreading pain
• Numbness or tingling
• Sudden weakness
• Swelling
• Pain that impedes basic movement
• Symptoms that feel new or unusual
Stopping therapy early is not a sign of failure. It is a measure to protect your health and support long-term progress.
(9) When You Should Call Prestige Medical & Physical Therapy

You should never manage confusion on your own. We encourage you to reach out whenever something feels unclear or soreness takes an unexpected turn. Early communication allows us to prevent setbacks and adjust your plan before pain intensifies.
Contact us if:
• Your pain feels sharp or electric.
• You cannot bear weight on a limb.
• You experience numbness or tingling.
• You notice swelling or redness.
• Your symptoms change in a concerning way.
• You feel uncertain about anything you are experiencing
Therapy is most effective when it functions as teamwork. You bring honesty, we bring expertise, and together we maintain steady, safe progress in your recovery.
A Closing Note of Reassurance
Soreness can feel unsettling, especially when pain has been present for years. We want you to understand that it is not a setback. It is your body responding to the work you are doing. It is your muscles reactivating, your joints finding space, and your nervous system learning that movement can be safe again.
Healing does not go unnoticed. It appears in tenderness and muscle fatigue, in effort, in the gradual return of strength, and in quiet confidence. Trust that process. Trust that you are not navigating it alone. We remain with you through every phase, providing steady care and close attention to how your body responds.
Soreness is a chapter, not the conclusion. Recovery requires time, and progress requires patience. Relief builds through small steps and consistent sessions. You can approach each next moment with confidence, and we will walk alongside you throughout your journey.
FAQs
Do I need to rest after every physical therapy session?
Yes, but you can get light rest, since gentle movement keeps soreness calmer and helps your body recover.
Can I work out on the same day as physical therapy?
You can only if the workout feels easy and does not trigger sharp or unusual pain.
Should I use heat or ice after my appointment?
You can, as ice helps when things feel swollen, and heat helps when things feel tight or stiff.
Can stress make my soreness feel worse?
Yes, because tension can heighten how your nervous system reacts to pain signals.

Can Physical Therapy Help You Avoid Surgery? Insights from Specialists
Many patients arrive with a mix of fear and hope, wondering if surgery is their only option or if clinical rehabilitation can still change the course of their condition. Prestige Medical & Physical Therapy welcomes individuals who have carried discomfort for months, along with the concern that their bodies may never regain steady function.
Our clinicians follow evidence-based evaluation standards, applying biomechanical analysis, targeted manual therapy, and progressive loading strategies to guide healing. Florida patients often want clear answers about whether physical therapy can help them avoid surgery, and for many, the outlook becomes hopeful once a tailored plan begins to take effect.
1) Why Non-Surgical Treatment Commonly Stands as the Clinically Preferred First Phase of Care
When evaluating a patient, the first question is whether function can be restored through less invasive measures. Skilled physical therapists focus on movement restoration, strengthening, and correcting patterns that drive pain. These strategies often lead to fewer complications, shorter recovery, and a quicker return to daily life.
Surgery remains essential for severe structural damage or neurological risk. For many degenerative and overuse conditions, structured rehabilitation improves joint mechanics, reduces pain sensitization, and rebuilds activity tolerance. Evidence-guided protocols with careful monitoring ensure decisions are data-driven and safe, preserving options while helping patients regain confidence in movement.
2) How Physical Therapy Guides a Safe and Effective Recovery Plan

Physical therapy reorients recovery from passive hope to active progress by giving patients specific tools that change how their bodies tolerate movement and load. At its heart, therapy is a staged process that restores capacity in a measurable way and helps people regain confidence in everyday tasks, from walking on sandy paths to lifting a grocery bag.
Core components and what they accomplish:
Progressive loading, where strength and endurance demands increase in planned steps, builds tissue tolerance and reduces flare-ups.
Movement retraining, which corrects faulty patterns that concentrate stress in one joint or tendon, spreads the load across healthier structures.
Neuromuscular control exercises that improve timing and coordination, lowering the risk of recurrent injury.
Graded exposure to feared activities, paired with pain education, which reduces sensitivity and restores normal activity without excessive guarding.
Manual techniques and hands on strategies that improve mobility and relieve painful stiffness when used selectively.
Functional integration, where gains in the clinic transfer to meaningful tasks and routines at home and work.
We also monitor progress with simple measures, for example, walking distance, sleep quality, and task-specific strength, so changes are visible and decisions are data-informed.
3) Conditions Where Rehabilitation Programs Can Help Avoid Surgery
In everyday practice we see patterns that matter clinically and practically, especially for people who prefer to avoid surgery if safe choices exist. American Academy of Orthopaedic Surgeons (AAOS) strongly recommends supervised exercise, land-based or aquatic, neuromuscular training, self-management programs, and patient education.
Basic conditions where therapy is frequently equal to surgery, with what the evidence says:
Degenerative meniscal tears, where randomized trials found exercise-based physical therapy noninferior to arthroscopic partial meniscectomy at five years, with many patients avoiding an operation when given a careful trial of rehabilitation.
Knee osteoarthritis, where systematic reviews consistently report that structured exercise programs reduce pain and improve function, and guidelines recommend exercise and education as foundational first-line care.
Rotator cuff tendinopathy and small to moderate tears, where several trials show meaningful improvements with supervised rehabilitation, and outcomes for pain and activity may be similar to surgery for selected patients at medium-term follow-up. Patient age, tear size, and activity goals shape the recommendation.
Many presentations of non specific low back pain, where conservative strategies led by therapists are the standard early approach; however, clinicians remain vigilant for red flags that change the pathway to urgent surgery. Guidelines emphasize measured, evidence-informed conservative care before operative options for most cases.
We translate this evidence into a clear trial of targeted rehabilitation, monitor objective progress, and keep surgical consultation available when recovery stalls or anatomic urgency appears, so patients in Florida can choose a path that protects function and aligns with their life.
4) When Surgery Remains an Important Option
Some paths to recovery begin with therapy and stay there; however, surgery remains the right choice for certain problems. We recommend operative care when structural damage is severe, when neurological signs progress, or when conservative measures have been given a fair, well-documented trial and function remains unacceptable. Examples include displaced fractures, large tendon ruptures in high-demand patients, and emergent spinal compression with evolving weakness.
We explain these realities with care so people in Florida understand the trade-offs, the urgency when it exists, and the ways surgery can restore anatomy that therapy cannot. Choosing an operation is rarely a failure; it is a reasoned step when anatomy, safety, and patient goals align.
5) What a Structured PT Program Looks Like for Patients Hoping to Avoid Surgery
A good program is more than sessions on a schedule; it is a coherent plan that progresses with measurable checkpoints. Below are the important ingredients we use and why each matters.
Initial assessment, including functional tests and clear patient goals, to create a baseline and identify red flags.
Individualized exercise prescription, with staged increases in load and complexity to rebuild strength safely.
Movement retraining sessions that address biomechanics relevant to the patient’s daily life, for example, gait on uneven sand or lifting grocery bags.
When stiffness prevents progress, manual therapy and targeted mobility techniques are used as an adjunct rather than a crutch.
Pain education and pacing strategies that reduce fear-driven guarding and increase activity tolerance.
Home program with practical instructions and simple progress markers, so gains translate into daily function.
Regular outcome reviews at planned intervals, using objective measures to inform adjustments to the plan.
This framework keeps care proactive and accountable, and it helps people see progress in ways that matter to their lives.
6) Signs Your Nonsurgical Treatment Plan Is Working

Progress is rarely dramatic overnight; however, there are clear, existent world signs that therapy is moving you toward recovery. We encourage patients to track simple markers that reflect both function and quality of life.
Look for improvements such as:
Increased ability to perform a previously limited task, for example, climbing stairs, gardening, or walking the block.
Reduced need for pain medication or fewer pain spikes with normal activities.
Better sleep quality because pain is less intrusive at night.
Greater confidence when returning to familiar activities, with fewer protective movement patterns.
Objective gains on strength or mobility tests recorded by your therapist.
When these markers shift, clinicians and patients can celebrate small wins while sustaining momentum toward larger goals.
7) When to Reevaluate Your Recovery Plan With Specialists
If measurable progress stalls despite adherence to a thoughtfully delivered program, it is time to reassess. We recommend a structured reevaluation after an adequate therapeutic trial, typically around 6 to 12 weeks depending on the condition; however, timing is individualized.
Reevaluation may include:
Repeating functional measures and comparing them to the baseline.
Discussing adherence, barriers, and realistic goal alignment.
Updating imaging or arranging a specialist consultation if anatomy or neurological status is in question.
Consider prehab, where therapy continues to optimize strength and mobility prior to a planned operation, improving surgical outcomes and recovery speed.
Framing reassessment as a collaborative checkpoint removes pressure, and it keeps the patient’s safety and preferences front and center.
Frequently Asked Questions
Q: Can physical therapy truly replace surgery for my condition?
A: For many degenerative and overuse problems, high-quality therapy can deliver outcomes similar to early surgery; however, the answer depends on the specific diagnosis, imaging, and personal goals.
Q: How long should I try PT before reconsidering options?
A: A practical benchmark is six to twelve weeks for most nonurgent conditions, though some problems require shorter or longer trials based on symptom severity and progress.
Q: What if therapy initially increases my pain?
A: Temporary increases can occur when tissues are challenged; however, therapists use graded exposure and close monitoring to distinguish helpful adaptation from harmful overload.
Q: Do I need imaging before starting therapy?
A: Not always. Many patients begin safe, progressive rehabilitation without advanced imaging, unless red flags or specific clinical concerns suggest it is necessary.
Q: How do I know I am safe to delay surgery?
A: Safety is determined by objective progress, absence of neurological deterioration, and shared decision-making with your care team. Preservation of function and absence of urgent signs usually make a therapy-first approach reasonable.
Q: Can PT help me if I ultimately choose surgery?
A: Yes, preoperative therapy strengthens tissues and improves mobility, which often leads to smoother recoveries and better outcomes after surgery.
Avoid Surgery and Recover Safely With Prestige Medical & Physical Therapy
We coordinate care across clinicians, communicate clearly about risks and expected timelines, and document progress so decisions rest on data, not anxiety.
Whether a patient remains on a nonsurgical path or moves toward an operation, our aim is to preserve dignity, maximize function, and reduce uncertainty. If you would like to talk through options or schedule an evaluation, contact Prestige Medical & Physical Therapy to arrange a consultation with one of our clinicians.
Read More →